2014
S. Kurugol, K. Kose, B. Park, J.G. Dy, D.H. Brooks, M. Rajadhyaksha.
“Automated Delineation of Dermal-Epidermal Junction In Reflectance Confocal Microscopy Image Stacks Of Human Skin,” In Journal of Investigative Dermatology, September, 2014.
DOI: 10.1038/jid.2014.379
PubMed ID: 25184959
Reflectance confocal microscopy (RCM) images skin non-invasively, with optical sectioning and nuclear-level resolution comparable to that of pathology. Based on assessment of the dermal-epidermal junction (DEJ) and morphologic features in its vicinity, skin cancer can be diagnosed in vivo with high sensitivity and specificity. However, the current visual, qualitative approach for reading images leads to subjective variability in diagnosis. We hypothesize that machine learning-based algorithms may enable a more quantitative, objective approach. Testing and validation was performed with two algorithms that can automatically delineate the DEJ in RCM stacks of normal human skin. The test set was composed of 15 fair and 15 dark skin stacks (30 subjects) with expert labellings. In dark skin, in which the contrast is high due to melanin, the algorithm produced an average error of 7.9±6.4 μm. In fair skin, the algorithm delineated the DEJ as a transition zone, with average error of 8.3±5.8 μm for the epidermis-to-transition zone boundary and 7.6±5.6 μm for the transition zone-to-dermis. Our results suggest that automated algorithms may quantitatively guide the delineation of the DEJ, to assist in objective reading of RCM images. Further development of such algorithms may guide assessment of abnormal morphological features at the DEJ.
2013
J. Sourati, K. Kose, M. Rajadhyaksha, J.G. Dy, D. Erdogmus, D.H. Brooks.
“Automated localization of wrinkles and the dermo-epidermal junction in obliquely oriented reflectance confocal microscopic images of human skin,” In Proc. SPIE 8565, Photonic Therapeutics and Diagnostics IX, Vol. 8565, 2013.
DOI: 10.1117/12.2006489
Reflectance Confocal Microscopic (RCM) imaging of obliquely-oriented optical sections, rather than with traditional z-stacks, shows depth information that more closely mimics the appearance of skin in orthogonal sections of histology. This approach may considerably reduce the amount of data that must be acquired and processed. However, as with z-stacks, purely visual detection of the dermal-epidermal junction (DEJ) in oblique images remains challenging. Here, we have extended our original algorithm for localization of DEJ in z-stacks to oblique images. In addition, we developed an algorithm for detecting wrinkles, which in addition to its intrinsic merit, gives useful information for DEJ detection.
2012
S. Kurugol, M. Rajadhyaksha, J.G. Dy, D.H. Brooks.
“Validation study of automated dermal/epidermal junction localization algorithm in reflectance confocal microscopy images of skin,” In Proceedings of SPIE Photonic Therapeutics and Diagnostics VIII, Vol. 8207, No. 1, pp. 820702-820711. 2012.
DOI: 10.1117/12.909227
PubMed ID: 24376908
PubMed Central ID: PMC3872972
2011
S. Kurugol, J.G. Dy, M. Rajadhyaksha, K.W. Gossage, J. Weissman, D.H. Brooks.
“Semi-automated Algorithm for Localization of Dermal/ Epidermal Junction in Reflectance Confocal Microscopy Images of Human Skin,” In Proceedings of SPIE, Vol. 7904, pp. 79041A-79041A-10. 2011.
DOI: 10.1117/12.875392
PubMed ID: 21709746
PubMed Central ID: PMC3120112
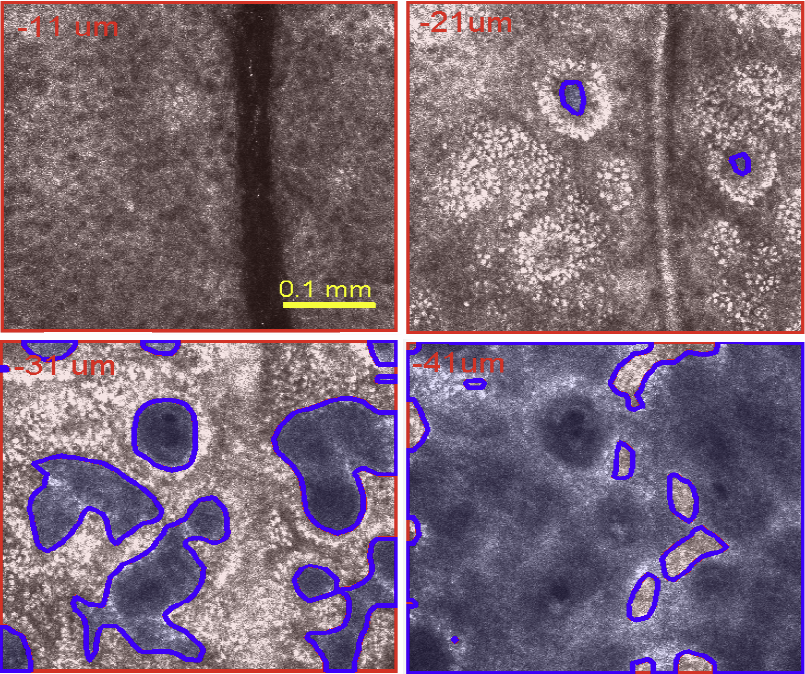
The examination of the dermis/epidermis junction (DEJ) is clinically important for skin cancer diagnosis. Reflectance confocal microscopy (RCM) is an emerging tool for detection of skin cancers in vivo. However, visual localization of the DEJ in RCM images, with high accuracy and repeatability, is challenging, especially in fair skin, due to low contrast, heterogeneous structure and high inter- and intra-subject variability. We recently proposed a semi-automated algorithm to localize the DEJ in z-stacks of RCM images of fair skin, based on feature segmentation and classification. Here we extend the algorithm to dark skin. The extended algorithm first decides the skin type and then applies the appropriate DEJ localization method. In dark skin, strong backscatter from the pigment melanin causes the basal cells above the DEJ to appear with high contrast. To locate those high contrast regions, the algorithm operates on small tiles (regions) and finds the peaks of the smoothed average intensity depth profile of each tile. However, for some tiles, due to heterogeneity, multiple peaks in the depth profile exist and the strongest peak might not be the basal layer peak. To select the correct peak, basal cells are represented with a vector of texture features. The peak with most similar features to this feature vector is selected. The results show that the algorithm detected the skin types correctly for all 17 stacks tested (8 fair, 9 dark). The DEJ detection algorithm achieved an average distance from the ground truth DEJ surface of around 4.7μm for dark skin and around 7-14μm for fair skin.
Keywords: confocal reflectance microscopy, image analysis, skin, classification
S. Kurugol, J.G. Dy, D.H. Brooks, M. Rajadhyaksha.
“Pilot study of semiautomated localization of the dermal/epidermal junction in reflectance confocal microscopy images of skin,” In Journal of biomedical optics, Vol. 16, No. 3, International Society for Optics and Photonics, pp. 036005--036005. 2011.
DOI: 10.1117/1.3549740
Reflectance confocal microscopy (RCM) continues to be translated toward the detection of skin cancers in vivo. Automated image analysis may help clinicians and accelerate clinical acceptance of RCM. For screening and diagnosis of cancer, the dermal/epidermal junction (DEJ), at which melanomas and basal cell carcinomas originate, is an important feature in skin. In RCM images, the DEJ is marked by optically subtle changes and features and is difficult to detect purely by visual examination. Challenges for automation of DEJ detection include heterogeneity of skin tissue, high inter-, intra-subject variability, and low optical contrast. To cope with these challenges, we propose a semiautomated hybrid sequence segmentation/classification algorithm that partitions z-stacks of tiles into homogeneous segments by fitting a model of skin layer dynamics and then classifies tile segments as epidermis, dermis, or transitional DEJ region using texture features. We evaluate two different training scenarios: 1. training and testing on portions of the same stack; 2. training on one labeled stack and testing on one from a different subject with similar skin type. Initial results demonstrate the detectability of the DEJ in both scenarios with epidermis/dermis misclassification rates smaller than 10% and average distance from the expert labeled boundaries around 8.5 μm.